“A lot of my patients exposed to substance abuse in utero require very frequent visits with multiple medical folks,” says JP’s doctor, Dianna Baker, a MaineGeneral pediatrician based in Winthrop. “It can be overwhelming for their caregivers.”
Along with the suffering an opiate-exposed baby endures comes extraordinary costs. Lisa estimates that medical care and therapy for JP surpassed $1 million before he turned 2. Like other children in the foster care system, JP was covered by MaineCare, a state and federally funded program for families and people with limited income.
With 4,877 babies born dependent on opiates or other drugs in Maine between 2013 and 2017, more and more babies like JP are being placed in the state’s custody.
“It’s been a growing population,” says Bette Hoxie with Adoptive Foster Families for Maine, which provides support and training for foster parents. “And some of these foster families go above and beyond. It takes a pretty special person to take on a medically fragile baby.”

Born at a low birthweight, JP had trouble swallowing. He aspirated or sucked milk into his lungs and then spit it up. He also suffered severe withdrawal symptoms from the opiates he was exposed to in the womb. Inconsolable, he rarely slept. His screams were high-pitched; his body trembled and then went rigid. He vomited, and had diarrhea and skin infections.
“He was in the hospital for two and half weeks and went home with his aunt and uncle, but they had another child and couldn’t handle him,” Lisa explains. “When I got him, the caseworker told me, ‘He’s four weeks old, cries and spits up a lot.’ ”
He had to be swaddled all the time. And if he wasn’t, he’d just shake and shake.”
— Lisa Hasch
Lisa, 33 at the time, was no stranger to challenges as a special education teacher at Monmouth Academy, but she had no experience caring for a baby with this many medical problems. JP continued to have withdrawal symptoms for the next four months.
“He had to be swaddled all the time,” Lisa recalls. “And if he wasn’t, he’d just shake and shake.”
Because JP had acid reflux, the infant spit up more food than he swallowed. At four weeks, he was only seven pounds. Despite his reflux medication, he struggled to drink formula.
“Feeding him took all day,” says Lisa, who had to bring JP to her summer job as the Monmouth waterfront director. “He never ate more than four ounces. Most time he took an ounce to two ounces. I was feeding him 16 to 17 hours a day to keep him at his weight.”
Over the next several months, along with frequent visits to his pediatrician for weight checks, JP would see many other specialists. He needed physical therapy to help him move his still-rigid left side. He saw a pulmonologist for his persistent cough and his asthma; a nutritionist to help formulate a liquid that would maintain his weight; a neurologist for his developmental delays.
A few days after his first birthday, JP was hospitalized.
“He was aspirating everything into his lungs,” Lisa says. “The nurse told me, ‘I don’t want to send you home. It’s not safe for this child to eat.’ ”
Left with no other options, a doctor inserted a gastrostomy tube through JP’s abdomen to deliver nutrition directly to his stomach.

“He was in the hospital for about a week,” recalls Lisa, who slept by JP’s side. “It was hard for him; he didn’t want to be in a bed. He wanted to run and play.”
A few weeks later, JP pulled his feeding tube out at 3 a.m. Lisa and her foster son rode in an ambulance to Maine Medical Center in Portland to have the tube reinserted.
“It’s been an emotional rollercoaster,” admits Lisa. “It’s exhausting, but you’re all they’ve got, so you do what you have to.”
Feeding him took all day. He never ate more than four ounces. Most time he took an ounce to two ounces. I was feeding him 16 to 17 hours a day to keep him at his weight.”
— Lisa Hasch
On a warm June afternoon, Lisa sits on her couch, with her rust-colored dog Cider sleeping beside her. A 9-month-old with round cheeks and bright blue eyes sits in the middle of a pile of plastic toys. A padded helmet covers his blonde hair to help reshape his skull.
“He was neglected, too,” Lisa says of her latest foster child. “He was left on his back so much he has flat-head syndrome.”
Down the hall, JP – now 2 – wakes from his nap, crying, “Mommm. Mommy.”
Lisa brings him back to the couch where she holds him on her lap. JP whimpers and she rubs his back. “What’s wrong, are you still sleepy?”
Blonde-haired with wary blue eyes, JP is still thin for his age. Though he is now able to eat solid food, he still must receive a daily dose of high-calorie and nutrient-rich formula food through his stomach tube so that he won’t lose weight. He continues to aspirate clear liquids, and cannot drink water or juice unless it has a powder that thickens it to a honey-like consistency.
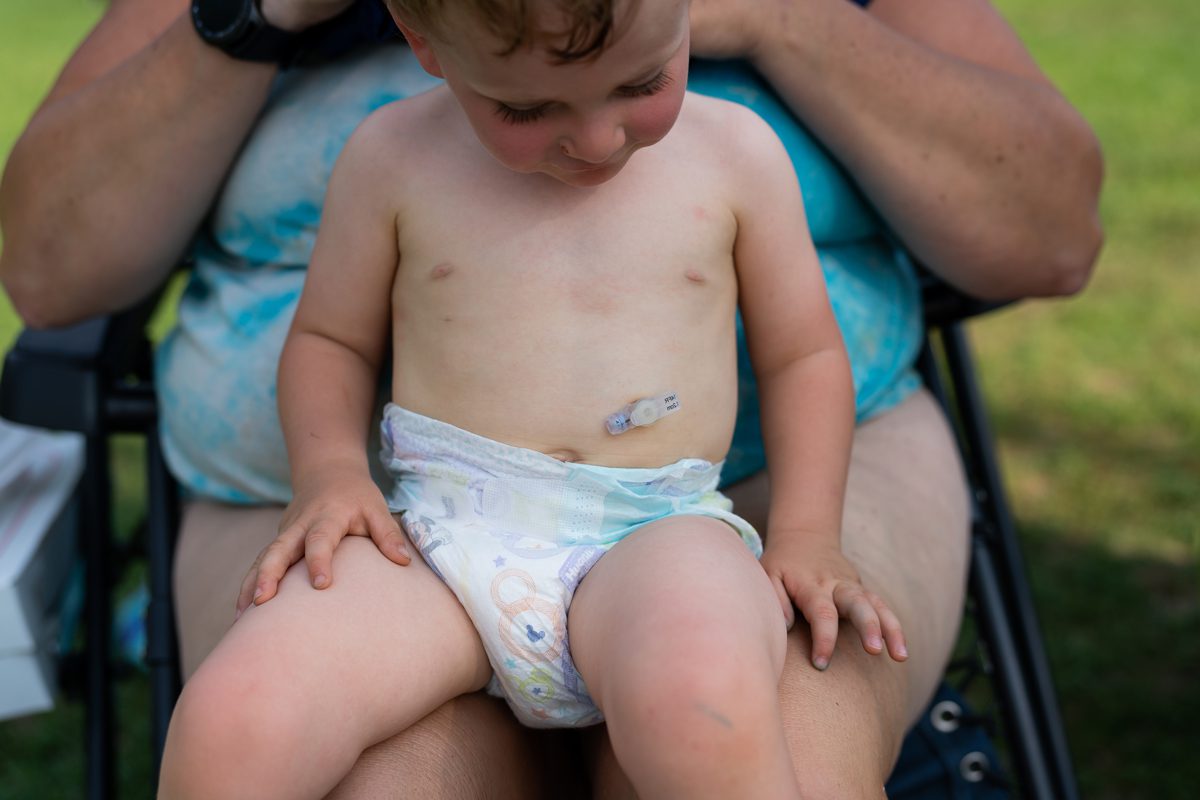
“He’s such a complicated kiddo,” Lisa says as JP slides off her lap and runs to pick up a ball. “I work so hard to get him to gain weight, and then we go to the doctor’s and he lost a pound. I cried that night. It’s frustrating; I just want him to move forward.”
JP has shed many tears, too. He cries when he sees his older brother drink chocolate milk, something he cannot have. He whimpers when he has to see a doctor, fearing what will happen next.
“This is trauma JP is going to face for the rest of his life,” explains Lisa. “It doesn’t go away. There are psychological aspects of it. Even now going to the doctors, he cries. It scares him. He had his weight checked recently and he freaked out.”
It’s been an emotional rollercoaster. It’s exhausting, but you’re all they’ve got, so you do what you have to.”
— Lisa Hasch
Doctors don’t have any answers on how long JP will continue to need his tube feedings that take a half hour. Nor do they know if he will ever be able to drink liquid without sucking it into his lungs.
“JP has been through so much,” Lisa says. “And it’s hard because in the back of my mind, I think, he doesn’t deserve this.”
But the 35-year-old mother has little time to dwell on what she cannot change.
This summer, Lisa adopted JP.
“It’s such a relief to know he is mine now,” she says, adding that she can now make all of JP’s medical decisions without the state’s approval. “But at the same my heart broke for the family he was leaving.”
Lisa knows JP’s birth parents would not be able to care for him, taking the 2-year-old to his multiple therapies and doctors’ appointments. She admits that sometimes she gets overwhelmed with the physical and emotional needs of her three boys.
“Do I enjoy taking my children to therapy appointments practically every day of the week after I have worked all day?” she said. “Not always, but I do it religiously because the end result is to help them get better at handling whatever it is that is a challenge for them.”
She also credits her family, friends, daycare and church for their support.
“They’re a godsend,” she says.
Sometime in the near future, Lisa hopes to adopt the toddler she calls ‘my little munchkin,’ who will become her third son. In many ways, she is like any other mom taking her boys apple picking, to county fairs and to the beach, but she knows her life will never be “normal” or routine. There will be many challenges to overcome, but she also is certain that she was meant to love and care for a baby that had nowhere else to go.
“JP was placed in my life because God knew that I could handle his many medical needs,” Lisa says. “While I have often become frustrated with things, I am reminded daily that he is happy and healthy and loved.”




