Not long after he was elected to the U.S. Senate six years ago, independent Sen. Angus King traveled throughout Maine listening to doctors, nurses, families and counselors share their concerns about the state’s opiate epidemic.
He learned about Maine’s high number of opiate overdoses, but what shocked him most was the number of drug-exposed babies.
“I can remember going to some of these rural hospitals where 10, 12 or 15 percent of the babies were drug affected,” King said. “It was like, OK, those are numbers you can’t ignore.”
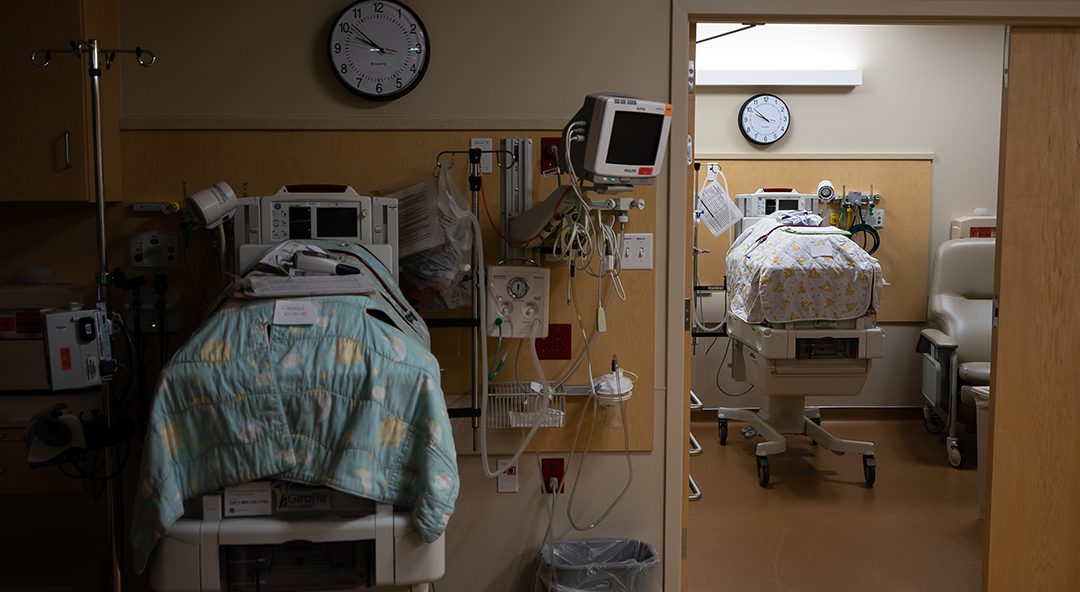
The senator also spent time in the neonatal intensive care unit at Bangor’s Eastern Maine Medical Center observing infants that were born opiate dependent.
One of the pieces that I sponsored and really worked on was making it OK for nurse practitioners and physician assistants to continue to administer medication-assisted treatment.”
— U.S. Sen. Angus King (I-Maine)
“It had a great impact on me … they are just so helpless, with tubes and wires. And it’s not the joyful place that it should be. It was an emotional experience.”
Sen. Susan Collins (R-Maine), elected in 1996, shared a similar story as she talked to families and doctors about the opiate crisis over the past four years.
“I was shown videos by Eastern Maine Medical Center of a baby who was born to an addicted mom versus a baby born to a mom without addiction,” Collins said. “The addicted baby just cried inconsolably. I kept thinking it was as if the poor little child couldn’t stand her own skin. She just couldn’t get comfortable, and she cried constantly.”
Those memories haunted King and Collins, prompting them to push for legislation and funding to reduce Maine’s high number of opiate-dependent infants.
After reading Pine Tree Watch’s “Born to Drugs” series, which reported that 4,877 drug-affected babies were born in the state between 2013 and 2017, overwhelming hospitals, the foster care system and other resources, the senators agreed that more needs to be done to alleviate the crisis.
“It was painful to read,” Collins said of the series, which was published in late November and December. “It’s going to be a real challenge, which is why we’ve got to figure a way to remove the stigma and expand treatment for these pregnant women.”
A significant majority of babies born in Penobscot County exposed to opiates were born to women who were excluded from medical coverage.”
— Dr. Noah Nesin, Penobscot Community Health Care’s chief medical officer
Along with advocating for more federal funding for Maine, Collins, King and U.S. Rep. Chellie Pingree (D-Maine) supported and sponsored bills in the Support for Patients and Communities Act that passed in October, which includes several laws focused on prevention and aid to communities and families overwhelmed by opiate addiction.
One of the most important aspects of the bill for King was making permanent a 2016 law that allowed nurse practitioners and physician assistants to prescribe buprenorphine, an opiate-replacement drug that eases cravings but does not produce a high. Previously, only doctors could prescribe the drug. But the 2016 law included a stipulation that nurse practitioners and physician assistants would only be able to prescribe through 2021.
“One of the pieces that I sponsored and really worked on was making it OK for nurse practitioners and physician assistants to continue to administer medication-assisted treatment,” King said. “We got it made permanent … That’s a big deal for Maine because of the rural nature of our state where you don’t have physicians in a lot of places. But there are 1,700 nurse practitioners in Maine, which I view as a huge asset.”
Dr. Elisabeth Mock, a Holden physician in rural Aroostook County, said changes in the law are making a difference.
According to the Maine Medical Association, the state has doubled the number of clinicians who can prescribe the opiate-replacement drug, increasing the number to 742, during the past four years.
Though the majority of those were doctors, Mock says she expects a growing number of nurse practitioners and physician assistants will offer the medication-assisted treatment over the next several months.
“In 2014, few people were talking about offering the medication-assisted treatment,” Mock said. “But now we’re seeing a lot more interest.”
Broadening the program, healthcare providers say, is especially important for pregnant women with opiate addiction. Women using illicit drugs have higher risks of fetal death and complications. To increase an infant’s chance for a healthy birth, many maternal caregivers prescribe buprenorphine, commonly known as Subutex and Suboxone.
But it can be difficult for women to find a doctor to treat them.
“Ideally, women would be on medication-assisted treatment prior to pregnancy,” said Dr. Mark Publicker, a Portland psychiatrist and longtime addiction specialist. “But there hasn’t been an easy portal for women to find someone, and if they aren’t insured and can’t get treatment, they’re going to be using street drugs until their fourth or fifth month of pregnancy.”
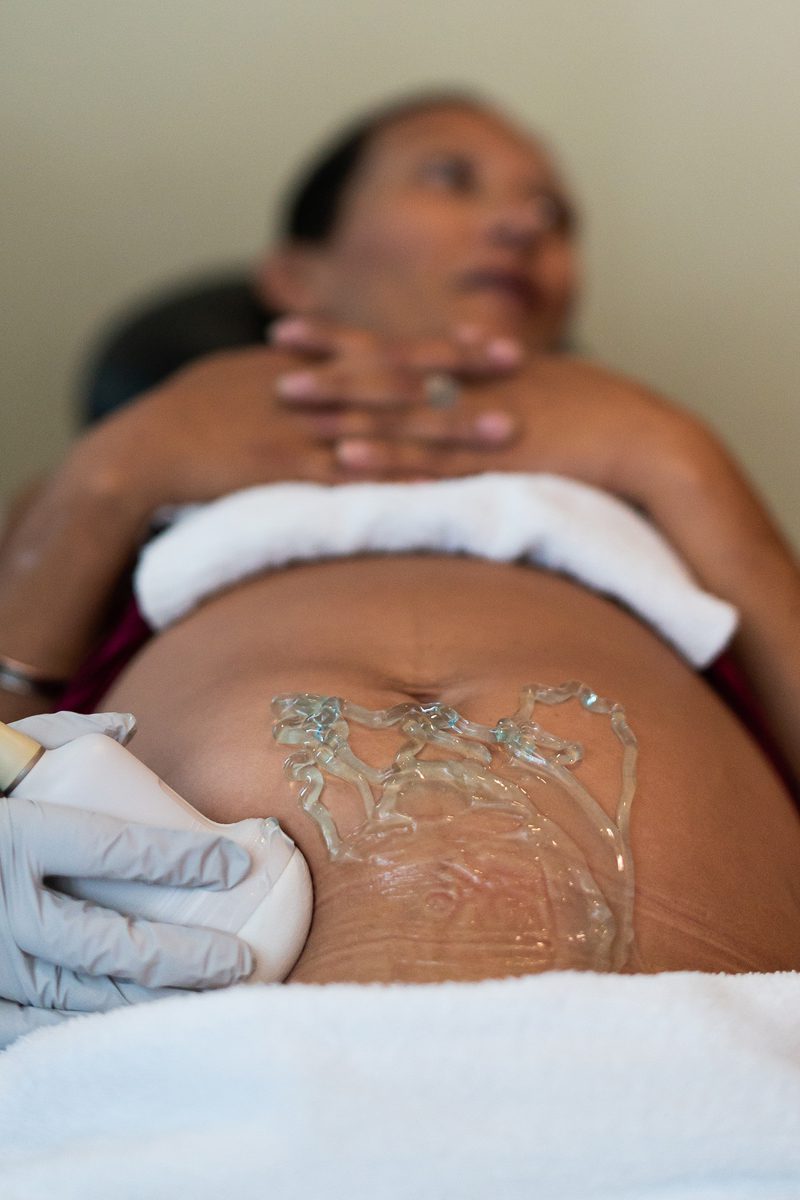
With Gov. Janet Mills’ immediate implementation of voter-approved Medicaid expansion upon taking office this month, 25,000 to 30,000 lower income people with substance-use disorders now will be able to access insurance, allowing them to get treated with buprenorphine.
Since last July, 6,000 people have applied for Medicaid but were unable to be enrolled while former Gov. Paul LePage fought the expansion in court.
Doctors specializing in treating women with opiate addictions say the expansion may help prevent unwanted pregnancies and reduce the state’s high number of opiate-dependent babies.
In Penobscot County, for example, where 666 drug-affected babies were born between 2014 and 2016, doctors are optimistic that Medicaid expansion will allow them to treat more women before they become pregnant. Once a woman is pregnant, she is eligible for Medicaid or MaineCare as it is commonly called. The ideal scenario, doctors say, is to provide medical care to women of childbearing age before they face an unwanted pregnancy.
“A significant majority of babies born in Penobscot County exposed to opiates were born to women who were excluded from medical coverage,” said Dr. Noah Nesin, Penobscot Community Health Care’s chief medical officer. “If they can get coverage prior to pregnancy, they have access to more options for contraception.”
Long-acting reversible birth control such as the intrauterine device (IUD), Nesin said, is far more effective for women with opiate addictions who are unlikely to be focused on taking birth-control pills every day.
The lack of medical and opiate treatment for pregnant women in rural communities outside of Bangor, contributes to Penobscot County’s high rate of opiate-exposed babies, he said. The expansion of insurance for low-income Mainers will offer them more alternatives.
“We know people who have medication-care coverage are more engaged in their own health,” Nesin said. “It allows women to stabilize their lives or get an education before they become pregnant.”
Courtney Allen – featured in PTW’s Born to Drugs series – found herself facing tough choices when she was using opiates and became pregnant at age 19. A nurse at an Augusta needle exchange told Courtney she and her unborn child would be safer if she began taking the opiate-replacement drug.
Now 25 and in recovery, Allen is a University of Maine student and a Family Drug Court mentor to other parents. When someone is struggling with opiate addiction, their focus is on survival, not birth control, Allen said.
Allen recently learned of a woman in the Augusta area who had contracted hepatitis from a dirty needle and could not afford the prescriptions to treat her illness.

“She was really sick and general assistance was helping her, but she couldn’t get the treatment she needed,” Allen said. “With the expansion, she would be eligible for MaineCare.”
And once a woman seeks help for hepatitis or decides she wants to be placed on an opiate-replacement drug, it opens the door to other opportunities, Allen said.
“Women can get access to counseling, HIV or hepatitis treatment and then birth-control options will come when they have a doctor,” said Allen.
With an average of 975 drug-affected babies born each year – nearly three a day – between 2013 and 2017, Maine has one of the highest rates of opiate-affected babies in the country, according to the U.S. Centers for Disease Control.
The surge in opiate-addicted pregnant women has challenged Maine’s hospitals, treatment centers and the foster care system, which saw a 45 percent increase in the number of children placed in state custody between 2012 and 2016.
Often these children end up being raised by their grandparents, Collins said.
“There’s been a huge increase in the number of grandparents raising their grandchildren that is directly tied to the opiate crisis,” said Collins. “In Maine, it increased 24 percent over a five-year period (between 2010 and 2015) … It can be incredibly difficult for someone who is retired and they think they’re going into their golden years, and all of a sudden they have an infant to raise.”
As part of the opioid package passed in October, Collins co-sponsored a law to create a national advisory council to support grandparents raising grandchildren. The council’s focus is to identify and share resources to help grandparents as they try to keep their families together.
“Our goal is to have a central place where grandparents can get information they need,” said Collins, who chairs the Senate Aging Committee. “To find out what kind of stipends are available to them, what kind of counseling, what kind of medical treatment. To suddenly find themselves raising young children once again often puts a terrible strain on the health of the grandparent.”
There’s been a huge increase in the number of grandparents raising their grandchildren that is directly tied to the opiate crisis. In Maine, it increased 24 percent over a five-year period (between 2010 and 2015) … It can be incredibly difficult for someone who is retired and they think they’re going into their golden years, and all of a sudden they have an infant to raise.”
— Sen. Susan Collins (R-Maine)
Last year, Congress appropriated $8.5 billion to fund more treatment, prevention and programs like the advisory council to support grandparents; Maine received $16.9 million, Collins said. But Collins and Congresswoman Pingree believe Maine should have received more money due to its high rate of overdose deaths.
Last September, the Substance Abuse and Mental Health Services (SAMHSA) – which provides information, services and research – used overdose data from 2016 when it awarded its Opiate Response Grants.
Delaware and Rhode Island, tied for the 10th highest per capita overdose rate, and each received $12.5 million. Ranked 11th in 2016 with 376 deaths, Maine received $4.4 million.
In 2017, Maine climbed to ninth highest in overdose rates nationally with 418 deaths. Had SAMHSA used the 2017 data, Maine would have received a much larger portion of the grant money. But because the U.S. Centers for Disease Control had not yet compiled a state-by-state comparison of the 2017 overdose deaths, Pingree said, Maine fell off a funding ‘cliff’ due to its 2016 11th place ranking.
“Under SAMHSA’s formula, based on the number of deaths per capita related to overdoses, the top 10 states received good amounts of money,” said Pingree, who serves on the congressional Appropriations Committee. “New Hampshire, which has similar demographics and similar issues (to Maine), got $22.9 million and Maine got $4 million. We’re trying to get the formula adjusted, so there isn’t this sort of cliff (effect).”
Though he is new to Congress – he just started his first term – U.S. Rep. Jared Golden (D-Maine) echoed Pingree’s concerns about Maine’s funding shares.
“Every doctor I’ve talked to, every healthcare professional that has dealt with issues of substance abuse disorder, has said we are right now in the midst of a growing epidemic, and you have to put emphasis on expanding treatment,” he said.
In particular, Maine’s high rate of opiate-dependent babies deserves more attention, Golden said. “Everyone can agree that there should be more funding and programs to treat drug-affected babies. This is all through no fault of their own, and we can all get behind doing a little bit more here.”
A Marine veteran who served two combat tours, Golden says he often falls back on his military training when faced with a problem.
“In the military, we’re taught stop the bleeding, then treat the wound,” Golden said. “Sadly, Maine has not made much progress (with the opiate epidemic). We’re still in the stages of trying to stop the bleeding.”




