While Maine struggles to obtain enough personal protective equipment for healthcare workers and supplies to provide critical care, the state must now grapple with a new concern as the spread of the coronavirus accelerates: where to move the sick when hospital beds fill up.
A single 250-bed federal medical station is all Maine has to expand its hospital capacity statewide, the Maine Monitor has confirmed with the Maine Emergency Management Agency. Used in New York following Hurricane Sandy in 2012, the second-hand medical station has no medical supplies and only limited durable medical equipment, including cots and hand-washing stations, yet it will be the backbone of the next phase of Maine’s response to the virus.
The Maine Center for Disease Control and Prevention intends to divide the medical station into 50-bed “modules” to be set up as alternate care sites to avoid overwhelming hospitals, Maine CDC head Dr. Nirav Shah said. The state will set up the first 150 beds at arena or auditorium-type facilities by next week.
“I hope we never need to use these sites, but we cannot afford to wait to find out. Building them now will ensure that if the need does arise, we will be prepared and Maine people will be cared for and Maine people will survive,” said Gov. Janet Mills on Tuesday during a joint press conference with the Maine CDC.

The Cross Insurance Arena in Portland will receive 100 beds to serve southern Maine, where the majority of the state’s cases have been detected in Cumberland and York counties. A second site with 50 beds will open at the Cross Insurance Center in Bangor.
There was still excess capacity in Maine’s hospitals to treat patients critically ill with COVID-19 as of Monday, Shah said at his daily press briefing. Of the 300 ICU beds in the state, 120 were available. There were also at least 268 available hospital ventilators.
COVID-19 is a respiratory illness caused by a novel strain of the coronavirus, which originated in Wuhan, China in late 2019 and has rapidly spread across the globe. The virus is spread person-to-person during periods of close contact when the respiratory droplets of an infected person’s cough or sneeze is inhaled or touches another person’s mouth or nose, according to the federal CDC.
While Maine hospitals still have available beds to treat patients with COVID-19, the preparation of alternate care sites is necessary now to prevent a deadly surge of ill patients that could overwhelm medical staff and compromise patient care, said Steven Michaud, president of the Maine Hospital Association.
The spread of the coronavirus is still in the acceleration phase nationwide, according to the federal CDC. Shah said on Tuesday that coronavirus cases in Maine have not yet peaked and the state may not know when case totals have peaked until days or weeks after the fact.
The Maine CDC is also continuing to plan with hospitals to open two additional alternate care sites in each eastern and western Maine, Shah said.
‘Umbrella in a hurricane’
Setting up the physical infrastructure of an alternate care site is only the first hurdle to lowering the patient load on Maine’s hospitals. Once opened, they will need to be staffed and stocked with medical supplies.
Following the H1N1 pandemic in 2009 that sickened thousands of Maine residents and hospitalized almost 250 people — the majority of which were children and young adults — Maine hospitals were asked to revise their surge plans. One of the concerns was that several locations selected by hospitals as alternate care sites prior to the pandemic were “impractical” or “outdated,” according to an after-action report by the Maine CDC. These sites were not disclosed in the report.

During the COVID-19 pandemic, state employees will manage the logistics and set-up of the alternate care sites, but hospitals will manage staffing and patient care within the geographic regions, said health and human services Commissioner Jeanne Lambrew on Tuesday. These include MaineHealth and Northern Light Mercy hospitals in Portland and Eastern Maine Medical Center and St. Joseph Hospital in Bangor.
“Because we want these sites to be totally linked with the healthcare systems there, we are working in earnest to figure out what their needs are, what type of patients should be there and what type of staffing is required. That is a work in progress,” Lambrew said.
MEMA will stock the sites with medical supplies “through the same channels that we are using for other medical facilities across the state,” said an agency spokeswoman Susan Faloon. No personal protective equipment came with the federal medical station.
MEMA is in the process of distributing three shipments of medical supplies from the federal strategic national stockpile to healthcare facilities statewide, after Maine exhausted its stockpile of personal protective equipment within two weeks of diagnosing its first positive case of COVID-19.
State and federal stockpiles of personal protective equipment have proven to be inadequate to respond to the coronavirus pandemic.
The availability of personal protective equipment continues to be a top concern of Maine hospitals as the facilities assist in the opening of the alternate care sites, Michaud said.
“At the state level and federal level you’ll hear, ‘we sent out a million things,’ well it’s out of context. A lot of what we hear from the federal government when they talk about that is all drops in the bucket,” Michaud said. “Maine CDC is doing a fabulous job in allocating and trying to make sure they achieve the best balance that they can, but (Shah) said it, ‘I’ve got an umbrella in a hurricane,’ and that’s the truth.”
Hospital preparations
 Maine hospitals have trained for the metaphorical “hurricane” in coordinated surge drills — the most recent of which occurred in January, said Maine CDC spokesman Robert Long.
Maine hospitals have trained for the metaphorical “hurricane” in coordinated surge drills — the most recent of which occurred in January, said Maine CDC spokesman Robert Long.
Using the Freedom of Access Act, the Maine Monitor reviewed the past two quarterly reports submitted by the state’s new hospital preparedness coordinator All Clear Emergency Management Group to confirm that all state preparedness plans and drills had been completed.
The Maine Monitor found that the state’s pediatric surge plan had not yet been completed with a draft and validation exercise not due until April 30. Long confirmed that the state’s pediatric surge plan has not yet been validated.
There were 14 cases of COVID-19 in people under the age of 20 in Maine as of Tuesday. However, the average age of people infected by the virus has skewed older.
Barbara MacPike, infection preventionist for Mount Desert Island Hospital, said the last “large full-scale multi-agency training exercise” the Hancock County hospital participated in was in April 2019, but recent drills run by All Clear Emergency Management Group were “conducted very well, with very quick feedback to all participating institutions on what went well and areas for improvement.”
Nearly 20 other Maine hospitals did not respond to requests made over the last two weeks to comment on the quality of the drills.
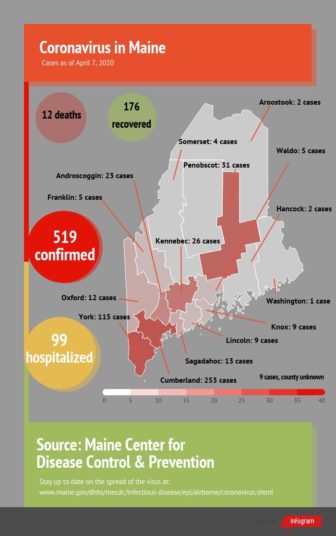
As of Tuesday, there were 519 people sick with COVID-19 in Maine, 99 of whom were hospitalized at some point during their illness, which is an increase of seven hospitalizations from Monday. During a pandemic, a surge in sick people is a question of when not if.
“One consistent feature important for preparedness planning is the rapid surge in the number of cases and their exponential increase over a very brief time, often measured in weeks. This will always result in a sudden sharp increase in the need for medical care,” according to Maine’s Pandemic Influenza Operations Plan.
Maine hospitals have already begun converting post-anesthesia care units, which would typically care for patients after surgery, into rooms capable of providing intensive care to expand in-hospital surge capacity, Michaud said.
York Hospital did not respond to a request for comment on its surge planning by press time. Maine Medical Center in Portland directed questions on when it was anticipated to exceed its capacity and need additional beds at an alternate care site back to the Maine CDC.
“The Maine CDC is coordinating surge planning statewide and, as such, they would be best positioned to speak to these issues,” John Porter, a spokesman for MaineHealth, said in an email on Monday.
Bracing for surge
President Donald Trump issued a Major Disaster Declaration in all 16 Maine counties on April 4 and a day later told the nation to brace for potentially “the toughest week” with many deaths expected due to the coronavirus.
Mills also asked the Trump administration to place the Maine National Guard under Title 32 status to aid in the state’s response to the coronavirus. The status change would allow Mills to order guard soldiers into full-time duty at the federal government’s expense.
As of last Friday, about 10 service members were on state active duty to assist full-time personnel in manning the National Guard’s joint operations center and augment their planning staff, Faloon said. A team of six National Guardsmen were inventorying medical supplies.
There have not been any large group or full unit activations, she said.
“Regardless of the status of that request, the Maine National Guard currently has the ability to act in state active duty at the Governor’s direction,” Faloon said.
Mills said on Tuesday she is directing the National Guard and MEMA to assist in the set-up of the alternative care sites in Portland and Bangor.
Already, the Maine National Guard has provided tents, HVAC and lighting to the Togus VA Medical Center for its external triage unit, as well as additional respirators for Bangor’s Northern Light Eastern Maine Medical Center and the Portland Fire Department.
In the past few weeks, the state has also recruited recently retired anesthesiologists and certified registered nurse anesthetists volunteers to bolster Maine’s workforce of 130 respiratory therapists.
While the state awaits additional resources to fight the virus, Mills requested Maine residents and visitors continue to stay home and socially distance themselves to slow the spread of the virus.
“What our future will look like — whether it is a best-case scenario or worst-case scenario or somewhere in between — that is all up to us,” Mills said.